Prevention of Mother-to-Child Transmission (PMTCT) of HIV is one of the primary focuses of HIV/AIDS prevention programs in low income nations. It is the centralized feature this week in USAID’s 5th Birthday campaign, due to its essential role in keeping children alive to their 5th birthday and beyond.
Key Measures
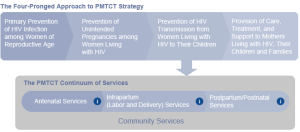
One of the key measures of effectiveness is how many are able to complete the PMTCT cascade: which should be initiated starting at antenatal care, to counseling and testing, through starting timely treatment, to returning to test the infant and follow-up care for the infant.[i] Antiretroviral therapy (ART) is effective in reducing rates of mother-to child transmission of HIV to low levels in resource-limited contexts but the applicability and efficacy of these programs in the field continue to be scarcely known.
Source: USAID/AIDSTAR One/ PEPFAR
ART and Protective Factors
It is important to note that PMTCT includes prenatal care, pregnant women receiving triple-drug ART coupled with exclusive breastfeeding after the infant is born. The longer and more comprehensive the treatment, the lower were the risks for transmission. Exclusive breastfeeding and triple-drug antiretroviral treatment (ART) are both protective factors, while unplanned pregnancies and mixed feeding are risk factors associated with MTCT. Close to two-thirds of the pregnancies among HIV-infected women were unplanned in South Africa according to a 2011 report: South Africa’s first national PMCTC impact evaluation. Results from this evaluation were presented at the Sixth International AIDS Society conference (IAS 2011) in Rome.
Another critical factor is the realization that providing ART treatments to mothers is the key turning point in their own survival. HIV is the leading cause of death for women of reproductive age worldwide and a major contributor to infant mortality. Once a woman is able to be properly diagnosed, her access to ART treatments will continue to keep her viral loads low, maintaining her own health. According to a recent study published in May of 2012 in The Lancet, CD4 count increased less in participants with pre-treatment drug resistance than in those without. Which means that at least three fully active antiretroviral drugs are needed to ensure an optimum response to first-line regimens and to prevent acquisition of drug resistance.
Improved access to alternative combinations of antiretroviral drugs in sub-Saharan Africa is warranted.[ii] We already know the research in linking the survival of the mother to the survival of her children. Thusly once again, mortality factors of mother and infant are inextricably linked.
Outreach is still needed
In one study many women presented too late for PMTCT, and about 20% of infants did not complete follow up. This suggests the need of targeted interventions that maintain the access of mothers and infants to prevention and care services for HIV.”[iii] In Nigeria, a study showing the Reduction of MTCT of HIV is possible with effective PMTCT interventions, including improved access to ARVs for PMTCT and appropriate infant feeding practices. Loss to follow up of HIV exposed infants is a challenge and requires strategies to enhance retention.[iv]
According to the WHO’s Global Health Sector Strategy on HIV/AIDS 2011-2015[v], Option B+ proposes further evolution—not only providing the same triple ARV drugs to all HIV-infected pregnant women beginning in the antenatal clinic setting but also continuing this therapy for all of these women for life. Important advantages of Option B+ include: further simplification of regimen and service delivery and harmonization with ART programmes, protection against mother-to-child transmission in future pregnancies, a continuing prevention benefit against sexual transmission to serodiscordant partners, and avoiding stopping and starting of ARV drugs. While these benefits need to be evaluated in programme settings, and systems and support requirements need careful consideration, this is an appropriate time for countries to start assessing their situation and experience to make optimal programmatic choices.”[vi]
South Africa, which has drastically declined its prevalence of PMTCT to under 4%, has these critical guidelines for all HIV Infected pregnant women[vii]:
- Receive routine antenatal care, including iron and folate supplementation.
- Be offered information on the availability of PMTCT interventions at all health care consultations, and not only when visiting the antenatal clinic.
- Be clinically staged and have a CD4 cell count taken on the same day as the HIV test is done, and preferably at the first ANC visit (or at the earliest opportunity).
- Be screened for TB, in line with the BANC.
- Be screened and treated swiftly for syphilis and other STIs, in line with BANC.
- Receive regimens to prevent mother-to-child transmission of HIV (PMTCT regimen) OR lifelong ART if CD4 cell count <350 cells/mm (ART regimen).
- Be offered appropriate PCP and TB prevention prophylaxis.
- Be counseled on safer sex, family planning, postnatal contraception and partner testing
For more information about USAID’s and PEPFAR’s efforts in PTCTC, visit: http://www.aidstar-one.com/focus_areas/pmtct
Additional Reading:
- Harvard’s AIDS Prevention Initiative in Nigeria:
- WHO: PMTCT Strategic Vision 2010-2015 (PDF)
- The Lancet: Prevention of mother-to-child transmission of HIV and the health-related Millennium Development Goals: time for a public health approach
- PMTCT Country Guidelines- PEPFAR, USAID, AIDSTAR One
[i] . http://www.aidsmap.com/South-Africas-PMTCT-programme-reduces-mother-to-child-transmission-to-under-4/page/1880446/
[ii] Hamers, Ralph, et al. Effect of Pretreatment HIV-1 drug resistance on immunological, virilogical, and drug resistance outcomes on first line antiretroviral treatment in Sub-Saharan Africa: a multicenter cohort study. http://www.thelancet.com/journals/laninf/article/PIIS1473-3099(11)70255-9/fulltext
[iii] Lucianna C. et al. Effectiveness of a Prevention of Mother-to-Child Transmission Programme in an Urban Hospital in Angola. PLoS One. 2012;7(4):e36381. Epub 2012 Apr 30. http://www.ncbi.nlm.nih.gov/pubmed/22558455
[iv] Anjoe et al, Reducing Mother-to-child transmission of HIV: findings from an early infant diagnosis program in south-south region of Nigeria, BMC Public Health. 2012 Mar 12;12:184. http://www.ncbi.nlm.nih.gov/pubmed/22410161
[v] The WHO’s “Global Health Sector Strategy on HIV/AIDS 2011-2015: Let’s do what’s right for everyone”: http://www.who.int/hiv/topics/mtct/en/index.html
[vi] Use of Antiretroviral drugs for treating pregnant women and preventing HIV infection in infants, WHO, April 2012: http://whqlibdoc.who.int/hq/2012/WHO_HIV_2012.8_eng.pdf
[vii] Clinical Guidelines, National Department of Health, South Africa, 2010: http://www.fidssa.co.za/images/PMTCT_Guidelines.pdf


[…] Site visited on August 20, 2005. Mouse here for Related SitesEvery Child Should Reach their 5th Birthday: Preventing Mother-to-Child Transmission of HIV This entry was posted in Uncategorized and tagged breast feeding, child transmission, hiv and […]